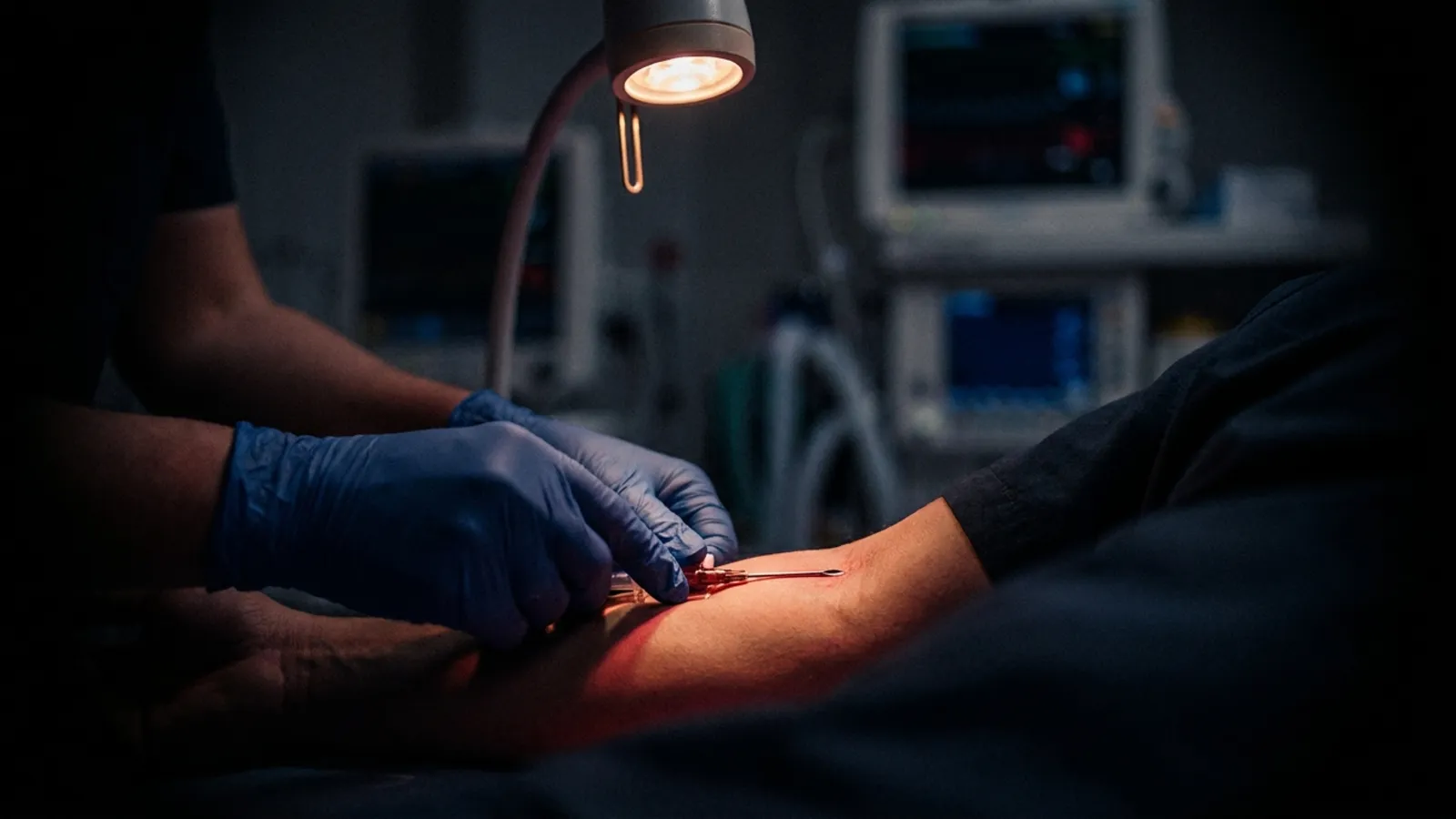
A blown vein happens when the vein wall is punctured through-and-through during cannulation, allowing blood and IV fluid to leak into surrounding tissue. The most common causes are too steep an insertion angle, advancing the needle after flash, applying excessive negative pressure on the syringe, and choosing fragile or unsupported veins. Prevention is mostly about three variables: angle, anchoring, and the moment you stop the needle.
You miss a stick. The patient flinches. A purple bruise appears under the skin within seconds. The vein you were just in is now firm, swollen, and useless. That is a blown vein. It happens to every clinician, but the frequency is highly trainable. This guide covers what actually causes blown veins, how to prevent them, and what to do in the moment when one happens.
What is a blown vein?
A blown vein, also called an infiltrated or hematoma-complicated vein, is a vessel whose wall has been punctured through both sides during cannulation. Blood escapes into the surrounding tissue, causing immediate bruising, swelling, and a firm, palpable mass. The vein typically becomes unusable for that attempt and often for several days afterward.
Blown veins differ from infiltration (where the catheter migrates out of the vessel and IV fluid leaks into tissue during infusion) and extravasation (the same migration with a vesicant or irritant). For a deeper guide on infiltration, see our IV infiltration signs and treatment article.
The seven most common causes of blown veins
Most blown veins trace to the same handful of technique faults. Knowing the list lets you self-diagnose what is happening on your own missed sticks.
1. Too steep an insertion angle. A 25 to 30 degree entry sends the needle through the back wall of the vein on the next millimeter of advance. The fix is a 10 to 15 degree entry, then drop nearly flat after flash.
2. Continuing to advance the needle after flash. Flash means the needle tip is in the vein. Pushing further sends it out the posterior wall. Hold the needle still after flash. Advance the catheter, not the needle.
3. Excessive negative pressure on a syringe draw. When drawing labs, pulling too hard on the plunger collapses the vein wall against the needle bevel and ruptures it. Slow, gentle pressure works. If blood return is slow, release and re-pull rather than yanking.
4. Choosing fragile, unsupported, or rolling veins without anchoring. Geriatric, dehydrated, and chemotherapy-exposed veins are more friable. A vein that is not held still rolls away from the needle and tears against the bevel during attempted entry. Use firm thumb traction below the planned site throughout the stick.
5. Tourniquet too tight or left on too long. Excessive tourniquet pressure causes hemoconcentration and stretches the vein wall. When the needle enters, the over-pressurized wall is more likely to rupture. Keep the tourniquet under 60 seconds and loose enough to maintain the radial pulse.
6. Fishing after a missed stick. Probing back and forth under the skin after a missed entry tears multiple vein segments. One missed stick becomes a multi-vein casualty. Pull back close to the skin (do not exit), redirect once cleanly, then withdraw if the second pass also fails.
7. Threading a catheter that meets resistance. If the catheter does not advance smoothly off the needle after flash, do not force it. The catheter may be against a valve, against the back wall, or in a tight bend. Pull back slightly, reassess, and either redirect or withdraw.
If you find yourself blowing veins repeatedly, the answer is not "be more careful." The answer is identifying which of these seven causes is your default failure mode and addressing it deliberately. Our companion guide on IV cannulation tips and tricks walks through each variable with a checklist you can use on your next shift.
Why some patients blow veins more easily
Patient anatomy and physiology determine baseline fragility. The same technique that succeeds on a healthy 30-year-old will blow a vein in a frail 85-year-old. Three categories of patient risk:
- Age and skin/vessel changes. Geriatric veins are thinner-walled and less elastic. A 25 degree entry that a 25-year-old vein tolerates fine ruptures an 85-year-old vein. See our IV cannulation in geriatric patients guide for technique modifications.
- Hydration status. Dehydrated veins collapse more easily under needle pressure and are harder to anchor. Our dehydrated patient IV access piece covers what to change when veins are flat.
- Medical history. IV drug use, repeated chemotherapy, multiple prior cannulations, dialysis, and corticosteroid use all weaken vessel walls. With these patients, the margin for technical error is much smaller.
When you know the patient profile is high-risk, slow down, double-check your angle, and consider whether ultrasound guidance would change the calculation. Our when to use ultrasound for IV access decision guide covers the threshold.
How to prevent blown veins (a checklist)
Use this short list before your next stick. Every item is something you control.
| Variable | Preventive action |
|---|---|
| Tourniquet | 4-6 inches above site, under 60 seconds, radial pulse intact |
| Vein selection | Forearm or dorsal hand first, avoid valves, avoid bifurcations |
| Anchoring | Firm thumb traction held throughout the stick, not just before |
| Insertion angle | 10-15 degrees on entry, drop to nearly flat after flash |
| Response to flash | Hold needle still, advance catheter only |
| Lab draws | Slow, gentle plunger pressure; release and re-pull if needed |
| Resistance during thread | Stop, do not force, reassess |
| Failed attempt | Withdraw to skin level, redirect once, then new site |
| Patient profile | Adjust technique for age, hydration, history; consider ultrasound |
Bottom line: Prevention is the cheapest intervention in IV cannulation. Most of these adjustments take less than a second to implement and prevent the cascade of pain, lost trust, and second attempts that come with a blown vein.
What to do when a vein blows during your attempt
Blown veins happen even with perfect technique. Recovery matters more than perfection.
- Withdraw the needle and apply firm pressure to the site for at least 60 seconds (longer if the patient is on anticoagulants). Pressure limits hematoma size and accelerates resolution.
- Apply a cold compress to the area for 10 to 15 minutes if available. Vasoconstriction reduces continued bleeding into tissue.
- Document the attempt in the patient's chart: site, gauge, what happened, and any patient response.
- Communicate with the patient. Acknowledge that the vein blew, briefly explain (without medical jargon) what that means, and let them know what comes next. Patient trust is built or lost in this moment.
- Choose a new site that drains independently. Avoid the same arm if possible, and never the same vein distal to the blown segment (the IV would infuse into the area of compromised vessel integrity).
- Reset before the next attempt. Take one slow breath, drop your shoulders, name the variable that caused the failure, and start the next stick deliberately. Our psychology of IV insertion article covers the mental reset in depth.
If you have already blown two veins on the same patient, the answer is almost always "stop and call." Continuing past two failed attempts is rarely the right move. A more experienced provider, a different vascular access strategy, or escalation to ultrasound or central access usually produces a better outcome than a third attempt.
What to tell the patient (and what not to)
How you communicate after a blown vein affects the patient's anxiety, their trust in you, and their willingness to let the next provider near them. A few principles:
- Acknowledge it directly. "That vein didn't cooperate" or "I'm going to need to try a different spot" is honest and brief. Avoid pretending nothing happened.
- Explain what it means in plain language. "The vein collapsed" or "we hit a small bruise" works. Avoid medical jargon like "hematoma" or "infiltration" unless the patient asks.
- Tell them what is next. Predictability reduces anxiety. "I'm going to put pressure here for about a minute, then we'll find a better spot on your other arm."
- Do not blame the patient. Saying "you have hard veins" or "your veins are rolling away" makes the patient feel responsible for a clinical event that is not their fault. The veins are what they are. Your job is to adapt.
- Do not over-apologize. A brief "sorry about that" is fine. Repeated apologies make the patient more anxious about the next attempt.
The clinicians patients ask for by name are the ones who recover gracefully when something goes wrong, not the ones who never miss.
What causes a blown vein during IV insertion?
A blown vein during IV insertion is most often caused by puncturing through the back wall of the vein, which happens when the insertion angle is too steep, when the needle keeps advancing after flash, or when the vein is not properly anchored with thumb traction. Patient factors like age, hydration, and medication history determine baseline vein fragility, but technique controls almost all preventable cases.
Why do my IVs keep blowing?
If your IVs keep blowing, the cause is usually one of three repeating technique faults: too steep an insertion angle, advancing the needle after seeing flash, or insufficient vein anchoring. Identify which one is your default failure mode by reviewing your last 5 to 10 missed sticks with an experienced colleague or instructor. Solo self-correction rarely works because the technique fault is invisible from inside the procedure.
Can a blown vein cause permanent damage?
Most blown veins resolve within 7 to 14 days with bruising and tenderness as the only lasting signs. Permanent damage is rare but possible if a large hematoma compresses surrounding nerves, if extravasation of a vesicant medication occurs, or in patients with bleeding disorders. Notify the provider if pain worsens, if the area becomes hard or hot, or if the patient develops numbness or motor changes downstream from the site.
How long does a blown vein take to heal?
A blown vein typically takes 7 to 14 days to fully heal in healthy adults, with visible bruising resolving over the first 5 to 10 days. Older patients, those on anticoagulants, and patients with vessel-compromising medical histories may take longer. The vein itself can usually be re-cannulated proximal to the blown segment after the bruising softens, though most clinicians choose a different vessel for at least one cycle.
Can I prevent blown veins entirely?
You cannot prevent blown veins entirely, but you can dramatically reduce the rate. Most experienced providers blow veins at well under 5 percent of attempts, while clinicians with technique faults can run 15 to 25 percent. The difference is rarely talent. It is structured feedback, deliberate practice, and identifying which of the seven common causes is the recurring fault in your own routine.
Ready to blow fewer veins?
The clinicians who blow the fewest veins are the ones who got real-time correction during their first 50 sticks. VeinCraft Academy's Level 1: The Method ($199) is built around that principle: 8 hours, class size of 10, credentialed clinical instructors observing your technique on live patients and correcting the angle, anchor, and post-flash pause that prevent most blown veins. Level 2: The Craft ($299) extends into hard-stick scenarios where blown-vein risk is highest.
Enroll now and start the next shift with technique your patients will feel.
VeinCraft Academy is a mastery-focused IV cannulation training program for healthcare professionals. All instruction is delivered by credentialed clinicians with active field experience. VeinCraft Academy is a RevivaGo Company.