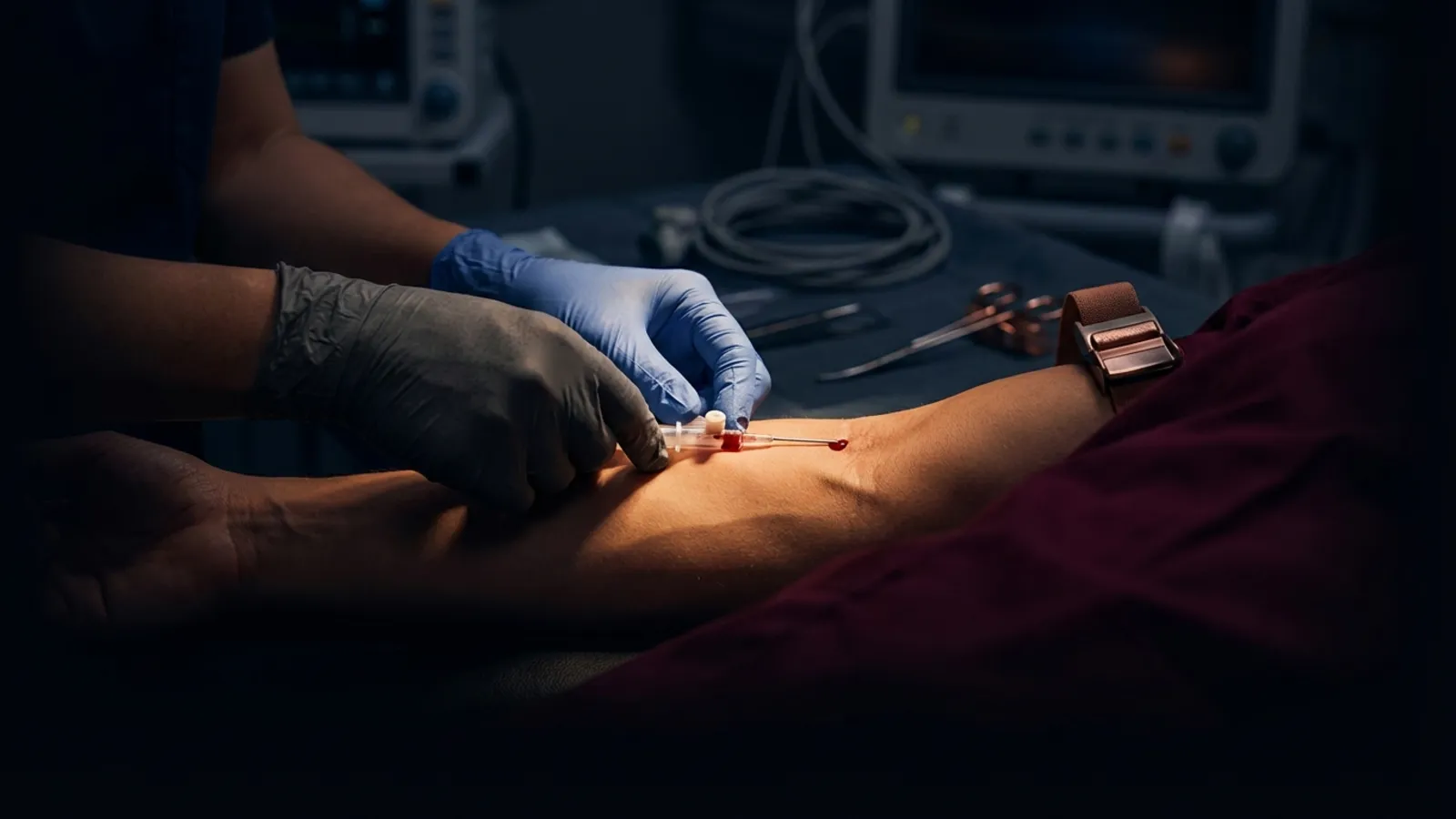
IV cannulation in geriatric patients requires modified techniques to account for fragile vein walls, thin skin, reduced subcutaneous tissue, and age-related vascular changes that make standard insertion approaches more likely to fail. According to a systematic review published in the Journal of Clinical Nursing, approximately 30% of hospitalized adults experience difficult intravenous access, and elderly patients are disproportionately represented in that group due to the cumulative effects of aging on vascular integrity.
If you work in a hospital, home health, or long-term care setting, elderly patients are not the exception. They are most of your IV starts. And the techniques that work reliably on a well-hydrated 30-year-old with visible veins will fail you on an 82-year-old with paper-thin skin and vessels that roll at the slightest contact.
This guide covers the specific modifications that make geriatric IV access more reliable, from site selection to insertion technique to post-insertion monitoring.
Why geriatric veins behave differently
Understanding what aging does to the vascular system changes how you approach cannulation. These are not just "difficult veins." They are structurally different from the veins you practiced on during training.
Vein wall fragility. Aging reduces the collagen and elastin in vein walls, making them thinner and less resilient. A vein that would tolerate a standard insertion in a younger patient may rupture under the same catheter pressure in an elderly patient. According to research published in the Australasian Journal on Ageing, peripheral IV catheter complications are significantly more common in older hospital inpatients, with fragile vasculature identified as a primary contributing factor.
Loss of subcutaneous tissue. As subcutaneous fat decreases with age, veins lose the supportive tissue that anchors them in place. The result is veins that sit closer to the skin surface (which sounds like it should be easier) but shift laterally when contacted by a catheter tip. This is the classic rolling vein problem, amplified by age-related tissue loss.
Skin integrity changes. Elderly skin is thinner, drier, and tears more easily. Aggressive traction during vein stabilization can cause skin tears before you even attempt insertion. Repeated tourniquet application can bruise fragile tissue.
Reduced venous compliance. Atherosclerosis and calcification stiffen vein walls over time. Stiff veins do not dilate well with tourniquet application, which reduces the engorgement you rely on for palpation and visualization. The tourniquet that plumps veins beautifully on younger patients may barely change vein diameter in an elderly patient.
Valve proliferation and tortuosity. Elderly veins often have more pronounced valves and a more tortuous (winding) path. Catheter advancement can catch on valves, and the winding path means the catheter may not thread smoothly even after a clean puncture.
Site selection for elderly patients
Site selection matters more in geriatric patients than in any other population. The wrong site increases your failure rate and complication risk significantly.
| Site | Geriatric Suitability | Notes |
|---|---|---|
| Forearm (mid to proximal) | Best choice | Veins are stabilized by underlying bones. Skin is usually thicker than hand or wrist. Less movement-related catheter migration. |
| Antecubital fossa (AC) | Good for short-term | Fewer valves, larger vein diameter. Use when you need reliable access quickly. Avoid for long dwell times due to flexion. |
| Dorsal hand | Use with caution | Veins are visible but extremely fragile in elderly patients. High risk of infiltration and skin tears. Reserve for short-term access when forearm is not available. |
| Wrist | Avoid if possible | Thin skin, heavy flexion, high complication rate in geriatric patients. Painful insertion site. |
| Upper arm (basilic/cephalic) | Alternative for difficult access | Deeper veins require ultrasound guidance but offer larger diameter and more stable positioning. |
Start your assessment at the forearm and work outward only if necessary. Resist the temptation to go for the visible hand vein that looks easy. In geriatric patients, visible hand veins are often the most fragile ones.
Modified insertion technique for fragile veins
Standard insertion technique needs several adjustments for elderly patients. Each modification addresses a specific age-related challenge.
Assess skin integrity first. Before applying a tourniquet or palpating, look at the skin. Note bruising from prior attempts, thin or papery texture, areas of skin tears or breakdown. This tells you how aggressive your technique can be.
Apply the tourniquet gently. Use light pressure. In many elderly patients, a blood pressure cuff inflated to just below diastolic pressure works better than a standard latex tourniquet. It distributes pressure more evenly and avoids the focal compression that can bruise fragile skin. If using a tourniquet, place it over a sleeve or thin cloth layer to protect the skin.
Use a shallow insertion angle. Drop your angle to 10 to 15 degrees, lower than the 15 to 30 degrees used for standard adult cannulation. Fragile vein walls are more likely to rupture with steeper angles because the catheter contacts the posterior wall sooner. A shallow approach gives you more control and distributes the insertion force along a longer segment of vein.
Apply gentle, steady traction. Anchor the vein with your non-dominant hand using consistent downward traction, not the firm lateral stretch that works on younger patients. Think steady pressure, not pulling. The goal is to hold the vein still without tearing the skin.
Watch for flash and stop. When you see blood return in the catheter chamber, pause. Confirm your position. Then advance the catheter slowly while withdrawing the stylet. Rushing the catheter advancement is the primary cause of through-and-through puncture in elderly veins. The vein wall cannot absorb the same forward force as a younger patient's vessel.
Advance by floating. After initial flash, connect a prefilled saline flush and advance the catheter while gently pushing saline. The fluid opens the vein ahead of the catheter tip, reducing friction against fragile walls. This "float technique" significantly reduces vein wall trauma during advancement.
Secure without pressure. Use transparent dressings applied gently. Avoid excessive taping. Consider a skin protectant barrier under the adhesive to prevent skin tears during removal. Ensure the hub is stabilized to prevent catheter movement.
The no-tourniquet method
For patients with extremely fragile veins, consider omitting the tourniquet entirely. This sounds counterintuitive, but it works in specific situations.
When elderly patients are on long-term corticosteroid therapy or blood thinners, their vessels are already thin-walled and prone to rupturing under minimal pressure. A tourniquet increases venous pressure, which over-distends these already compromised vessels. The moment you puncture the wall, the increased pressure causes blood to extravasate rapidly into surrounding tissue, resulting in a "blown vein" before you can thread the catheter.
When to try the no-tourniquet method:
- Patients on chronic corticosteroids with visibly fragile, bruised skin
- Patients with multiple blown veins from prior tourniquet-assisted attempts
- Patients whose veins are visible and palpable without a tourniquet
- Patients with significant bruising from previous IV attempts
Without a tourniquet, the vein stays at normal venous pressure. Puncture causes less trauma, and flash will still appear (though more slowly). You trade some vein distension for a significant reduction in rupture risk. For many geriatric patients, this tradeoff is worth it.
Medications that affect vein integrity
Elderly patients are often on medications that directly impact vascular integrity and IV success. Knowing what your patient takes before you pick up the catheter changes your approach.
Blood thinners (warfarin, heparin, DOACs). Anticoagulated patients bleed more from the puncture site and bruise extensively. Apply firm, sustained pressure after unsuccessful attempts. Expect hematoma formation even with clean sticks. This does not mean you did something wrong.
Corticosteroids (prednisone, dexamethasone). Long-term steroid use thins the skin and vein walls dramatically. These are the patients where skin tears during tourniquet application and veins blow on first contact. Use the no-tourniquet method and the gentlest possible traction.
Chemotherapy agents. Prior or current chemotherapy causes vein sclerosis and fibrosis. Previously used veins may be hard, cord-like, and non-compressible. Avoid these veins entirely and look for untouched sites. For patients with a history of extensive chemotherapy, ultrasound-guided access may be the most appropriate first-line approach.
Vasopressors and vasoactive medications. If the patient is on vasopressors, peripheral vasoconstriction will make vein access harder regardless of technique. Warming the extremity and allowing time for local vasodilation after tourniquet application can help.
Managing the anxious or confused elderly patient
Geriatric IV access is not only a technical challenge. The patient sitting in front of you may be anxious, confused, in pain, or all three. And their emotional state directly affects your access.
Anxiety triggers sympathetic nervous system activation, causing peripheral vasoconstriction. An anxious elderly patient's already marginal veins constrict further, dropping your success rate before you touch the catheter. Understanding the psychology of IV insertion applies to managing the patient's state, not just your own.
For anxious patients:
- Explain what you are doing at each step in simple, calm language
- Allow them to look away if they prefer
- Warm the extremity with a warm towel or blanket for two to three minutes before starting. This promotes vasodilation and signals to the patient that you are not rushing
- Acknowledge their discomfort. "I know this part isn't fun. I'm going to be as gentle as I can."
For patients with cognitive impairment or dementia:
- Minimize sudden movements near their hands and arms
- Speak in short, simple sentences. "I'm going to hold your arm gently."
- Have an assistant available to help stabilize the arm if the patient moves unpredictably
- Choose sites where the catheter can be secured away from their reach (forearm preferred over hand)
- Consider securement devices or mesh sleeves to prevent accidental removal
The providers who consistently succeed with geriatric patients are the ones who read the person before they read the vein. Spending an extra 30 seconds on patient rapport saves you from a failed attempt caused by a patient flinching at the wrong moment.
Post-insertion care and monitoring
Successful cannulation is only half the job. Geriatric IVs fail after insertion at higher rates than in younger patients due to fragile veins, accidental dislodgement, and infiltration.
Assessment frequency. Check the IV site every 1 to 2 hours at minimum. For elderly patients, especially those with altered sensation from diabetes or neuropathy, visual assessment is more reliable than asking "Does your IV hurt?" because they may not feel early infiltration signs.
Watch for delayed complications. Phlebitis risk is higher in elderly patients, particularly with dwell times beyond 72 hours. Redness, warmth, and tenderness along the vein path warrant catheter removal and restart at a new site.
Skin protection at removal. When removing the IV, use adhesive remover if available. Peel dressings slowly in the direction of hair growth. Apply gentle, sustained pressure to the site for at least two to three minutes, longer for anticoagulated patients. Even a clean removal can cause skin tears and bruising if you rush it.
When to escalate: ultrasound and vascular access teams
Two failed attempts is the standard threshold for escalation, and the Infusion Nurses Society Standards of Practice (2024 edition) recommend limiting insertion attempts to two per clinician. For geriatric patients, you might reach that threshold faster than with other populations, and that is fine. Recognizing when to escalate is a sign of good clinical judgment, not a failure of skill.
Consider escalation when:
- Two attempts have failed
- No palpable veins are found after warming and tourniquet application
- The patient has a history of difficult access documented in their chart
- Available veins are in high-risk locations only (hand, wrist)
Ultrasound-guided peripheral IV insertion allows you to visualize deeper veins that cannot be seen or palpated. For geriatric patients with depleted superficial access, the basilic or brachial veins in the upper arm often provide reliable, larger-caliber targets under ultrasound guidance.
If your facility has a vascular access team or IV therapy team, use them. These teams exist because difficult access is common and specialized skill reduces patient suffering and resource waste. VeinCraft Academy's Level 2: The Craft covers geriatric access, ultrasound-guided technique, and other special populations specifically because these skills require focused training beyond the basics.
How do you prevent blown veins in elderly patients?
Use a shallow insertion angle (10 to 15 degrees), apply gentle tourniquet pressure or use the no-tourniquet method, advance the catheter slowly after flash, and consider the float technique with a prefilled saline flush. Avoid aggressive traction on fragile skin. Choose forearm sites over hand sites when possible, and limit tourniquet application time to reduce venous over-distension. For patients on blood thinners or corticosteroids, expect increased fragility and adjust your force accordingly.
What gauge catheter is best for elderly patients?
A 22-gauge catheter is the standard first choice for most elderly patients. It is small enough to reduce vein trauma in fragile vessels while still accommodating most infusion therapies. For patients who need blood products or rapid fluid resuscitation, a 20-gauge may be necessary, but use it only when clinically required. A 24-gauge is appropriate for very fragile veins or when the only available access is a small hand vein. The Infusion Nurses Society recommends using the smallest gauge that will accommodate the prescribed therapy.
Why do elderly patients' veins roll?
Elderly patients' veins roll because of reduced subcutaneous tissue that normally anchors veins in position. As connective tissue thins with age, veins become more mobile within the surrounding tissue. When the catheter tip contacts the vein wall, instead of allowing puncture, the vein shifts laterally. This is worsened by dehydration (lower venous pressure makes veins softer and more collapsible) and loss of skin elasticity (reduced counterpressure from surrounding tissue). Traction with your non-dominant hand and proper vein anchoring are the primary countermeasures.
Should you use a tourniquet on elderly patients?
In most cases, yes, but with modifications. Apply lighter pressure than you would on younger patients, and consider placing the tourniquet over a cloth layer to protect fragile skin. Limit application time to reduce over-distension of fragile veins. For patients with extremely fragile veins, especially those on long-term corticosteroids or with multiple blown veins from prior attempts, the no-tourniquet method is a valid alternative. A blood pressure cuff inflated to just below diastolic pressure can also substitute for a traditional tourniquet, distributing compression more evenly.
Geriatric IV cannulation is a skill that rewards patience, preparation, and technique modification over speed. If you want to build confidence with elderly patients and other special populations through hands-on training with live patients, explore VeinCraft Academy's courses. Level 2: The Craft covers geriatric access, pediatric access, and ultrasound-guided technique, starting at $299, with mastery-based progression that means you advance when you can perform, not when the clock runs out.
VeinCraft Academy is a mastery-focused IV cannulation training program for healthcare professionals. All instruction is delivered by credentialed clinicians with active field experience. VeinCraft Academy is a RevivaGo Company.