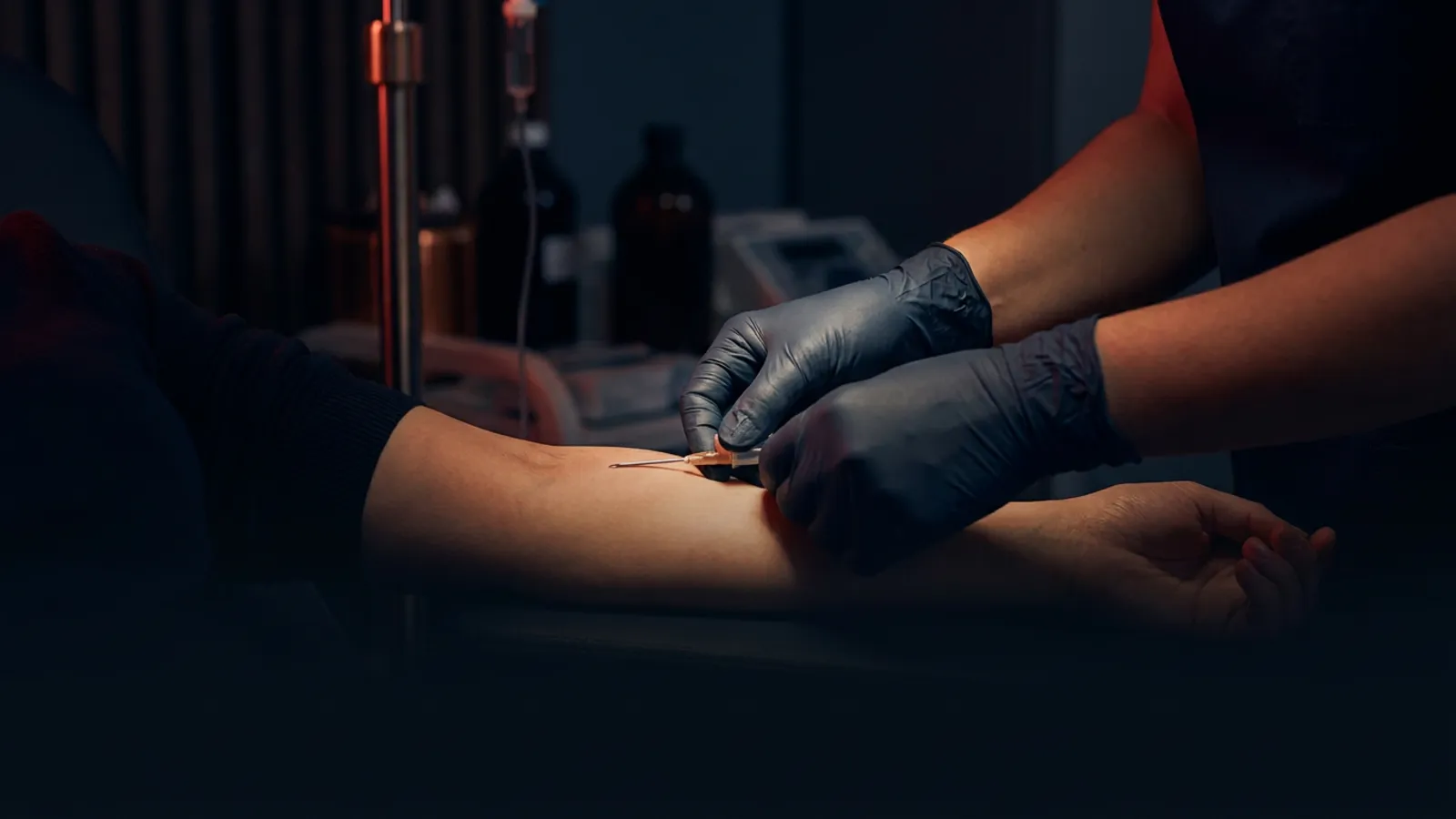
External jugular (EJ) IV access is the cannulation of the external jugular vein for peripheral venous access when standard upper-extremity sites have failed or are unavailable. It is a peripheral procedure, not a central line. The Infusion Nurses Society supports its use in acute and emergency settings, and a competent RN or paramedic can perform it under institutional protocol.
EJ access is the skill that often separates the provider others escalate to from the one who calls for the team. When peripheral attempts fail and the patient needs access now, the provider who can confidently identify, prep, and cannulate the EJ vein keeps the resuscitation moving. This guide covers the anatomy, indications, contraindications, technique, scope of practice considerations, and what published research says about success rates.
What is external jugular IV access?
EJ IV access uses a standard peripheral IV catheter inserted into the external jugular vein, which sits in the lateral neck and drains into the subclavian vein. It is classified as peripheral because the catheter tip stays in a peripheral vein, not in the central circulation. That distinction matters for scope of practice, dwell time, and infection control protocols.
The Infusion Nurses Society (INS) and the Journal of Emergency Nursing both recognize EJ peripheral IV catheters (EJ PIVs) as an established alternative for patients with difficult vascular access. Use should be temporary, with an alternative access site identified as soon as the patient is stable enough to allow it.
Anatomy of the external jugular vein
The external jugular vein runs superficially from the angle of the mandible down to the middle of the clavicle, where it joins the subclavian vein. Its location is what makes it accessible without imaging and what makes it visually obvious during patient positioning.
Three anatomical points matter for safe cannulation:
- Superficial position. The EJ sits above the sternocleidomastoid muscle, well lateral to the carotid artery and internal jugular vein. The risk of arterial puncture or pneumothorax that exists with internal jugular or subclavian access is functionally absent here.
- Visualization with positioning. The vein engorges and becomes visible when the patient is supine or in mild Trendelenburg, with the head turned to the contralateral side. Light supraclavicular pressure or a brief Valsalva maneuver enhances distension.
- Shallow course. Because the EJ runs just under the skin, the insertion angle has to be flatter than what you would use on a forearm vein. A standard 30-degree approach will usually overshoot.
Understanding the anatomy first is what makes the technique repeatable. Our vein anatomy for IV cannulation guide covers the broader vascular map; this article zooms in on the EJ specifically.
When to use EJ IV access (indications)
The Infusion Nurses Society supports EJ PIV use in two clinical contexts: acute care when other peripheral sites are unavailable, and emergency situations when access is time-critical. Specific indications include:
- Cardiac arrest and peri-arrest states when peripheral upper-extremity access has failed or cannot be quickly obtained
- Hemodynamic compromise requiring rapid fluid resuscitation or vasoactive medication delivery
- Documented difficult vascular access (DIVA) after multiple failed attempts at standard sites by competent providers
- Patient profiles that predict peripheral failure: severe hypovolemia, IV drug use history with sclerosed peripheral veins, vasculopathy, severe obesity with non-palpable upper-extremity veins, dialysis patients with preserved-vein protocols
- Bridge access while awaiting central line placement by a provider with appropriate scope and equipment
For patients who have already had two failed attempts at peripheral upper-extremity sites by a competent provider, our failed IV attempt protocol covers the structured escalation pathway. EJ is one of the options on that decision tree, alongside ultrasound-guided peripheral IV and intraosseous access.
Contraindications and patient selection
There are no absolute contraindications to EJ cannulation, but several relative contraindications should rule it out in favor of a different approach.
| Relative contraindication | Why |
|---|---|
| Cervical spine precautions | The patient cannot be positioned with head turn |
| Inability to lie flat or remain still | Positioning is essential and movement causes catheter displacement |
| Neck trauma or burns at the insertion site | Tissue compromise raises infection and bleeding risk |
| Active infection at the planned site | Standard infection control rules apply |
| Significant neck mass effect (goiter, lymphadenopathy, hematoma) | Anatomy is distorted and risk-benefit shifts |
| Severe coagulopathy with no central line backup plan | Hemostasis at the puncture site may be difficult |
If any of these apply, do not force the EJ. Escalate to a vascular access team, ultrasound-guided peripheral IV, or intraosseous access depending on the clinical urgency.
How to cannulate the external jugular vein
The technique below assumes you have institutional approval, completed competency training, and a documented EJ scope of practice. If you have not, this is reading material, not a procedural reference.
- Position the patient. Place the patient supine with mild Trendelenburg if hemodynamics allow. Turn the head to the contralateral side. Apply gentle supraclavicular pressure or ask a cooperative patient to perform a brief Valsalva maneuver to engorge the vein.
- Identify the vein. The EJ should appear as a visible cord crossing the sternocleidomastoid from the angle of the jaw to the middle of the clavicle. If it is not visible after positioning, do not blind-stick. Reposition or escalate.
- Prep the site. Apply 2% chlorhexidine gluconate (or 70% isopropyl alcohol if chlorhexidine is contraindicated) with friction for 30 to 60 seconds. Allow it to air dry for up to 1 minute. Do not blow on it or wipe it.
- Anchor and tense the vein. Use your non-dominant index finger to apply traction below your planned insertion site, stabilizing the vein along its long axis. The EJ rolls under the skin like a cooked spaghetti noodle without tension.
- Insert at a shallow angle. Use a 10 to 15 degree angle, bevel up. The vein is millimeters under the skin. A 30 degree angle that works on a forearm vein will pass through the EJ and into deeper tissue.
- Confirm and advance. Watch for flash. Note that the EJ runs at lower pressure than peripheral arm veins, so flash may be slow or muted. Drop the angle further to nearly parallel before threading. Advance the catheter off the needle in one smooth motion.
- Verify with saline flush. Flash alone is not enough confirmation in the EJ. Aspirate first, then flush with 5 to 10 mL of saline. The flush should be smooth, with no resistance, swelling, or ipsilateral facial pain.
- Secure for movement. The neck moves more than the arm. Use a transparent dressing, tape across the catheter hub, and a strain-relief loop. Document the dwell limit per institutional protocol.
If imaging is available and you are credentialed, ultrasound visualization of the EJ before puncture is reasonable and may improve first-attempt success. Our when to use ultrasound for IV access guide covers the broader decision flowchart.
EJ IV vs. central line: which is the right escalation?
Choosing between an EJ peripheral catheter and central venous access depends on the clinical urgency, the provider scope in the room, the planned therapy, and the duration of access required.
| Access option | Best for | Time to obtain | Provider scope |
|---|---|---|---|
| EJ peripheral IV | Emergent peripheral access when forearm sites fail; bridge to definitive access | 2 to 5 minutes | RN, paramedic with documented competency |
| Ultrasound-guided peripheral IV (USGPIV) | Difficult-access patients with deeper but accessible peripheral veins | 5 to 15 minutes | RN or paramedic with USGPIV training |
| Central venous catheter (IJ, subclavian, femoral) | Sustained vasoactive infusions, multiple infusates, weeks of therapy, central venous pressure monitoring | 15 to 30 minutes | Physician, advanced practice provider, or specially credentialed RN |
| Intraosseous (IO) | True emergency with no vascular access window | Under 1 minute | RN or paramedic with IO training |
Bottom line: EJ access is faster and less invasive than a central line and serves as a bridge to definitive access in most acute scenarios. It is not a substitute for a central line when the patient needs prolonged vasoactive support, multiple incompatible infusates, or central pressure monitoring. Use it for what it is, then escalate.
Scope of practice considerations
EJ cannulation by RNs and paramedics is governed at three levels: state board, institutional protocol, and individual competency documentation. All three must align before you do the procedure.
- State board. Most state boards of nursing, including Arizona, defer to facility policy and individual competency for EJ scope. The Nevada State Board of Nursing and others have issued advisory opinions explicitly placing EJ cannulation within RN scope when the nurse has documented training and demonstrated skill. Check your specific state board's advisory opinions before performing the procedure.
- Institutional protocol. Your facility must have a written policy authorizing EJ peripheral IV insertion by your role. The policy typically specifies indications, contraindications, required training, who supervises initial competency, dwell limits, and documentation requirements.
- Individual competency. The Infusion Nurses Society standard requires documented training, a supervised initial insertion or skills lab demonstration, and ongoing competency verification. Do not rely on a one-time class. Recertify on the schedule your institution sets.
For paramedics, EJ access is generally within Advanced Life Support scope under most state EMS protocols, but the same triple alignment applies: state EMS office, agency protocol, and individual training. Mobile IV providers operating outside a hospital should not perform EJ cannulation under most consumer mobile IV scopes; the indication for EJ is hospital-grade emergent access, not elective hydration.
Success rates and what the research says
Published data on EJ cannulation outcomes is most useful when it isolates the operator skill level.
According to a prospective observational study of junior clinicians published in the Journal of Contemporary Clinical Practice, EJ cannulation achieved 79% overall success across two attempts and a 62% first-attempt success rate, with a mean cannulation time of 148 seconds and a mean of 1.5 attempts per successful insertion. Complications were minor and rare: insertion-site swelling occurred in 3% of attempts and catheter malposition in 1%, with no arterial puncture, pneumothorax, or insertion-site infection reported.
In pediatric populations, a 2023 BMC Pediatrics study reported a 90.04% catheterization success rate via the EJ approach, with a 93.75% success rate in children younger than one year old, suggesting the technique is feasible across age groups when the operator is appropriately trained.
For experienced operators with structured training and high-volume practice, first-attempt success rates well above 80% are reported in case series and clinical experience. The 62% junior-clinician baseline is the relevant benchmark for new EJ providers, with the trajectory toward 80%+ following the same deliberate-practice patterns we cover in our guide on improving your IV start success rate.
Common pitfalls and how to avoid them
The mistakes most often made on EJ cannulation are not the same mistakes made on forearm IVs. Five pitfalls account for most failed attempts.
- Insertion angle too steep. A 25 to 30 degree angle that works on the antecubital fossa overshoots the EJ. Drop to 10 to 15 degrees and stay there.
- Inadequate vein engorgement. Skipping the head turn, Trendelenburg, or supraclavicular pressure leaves a flat vein that you cannot see and cannot anchor. Position the patient before you reach for the catheter.
- Failure to anchor. The EJ rolls more than a forearm vein because the surrounding tissue is loose. Anchor below the insertion site with firm thumb traction along the long axis of the vein.
- Aggressive advance after flash. The EJ runs at lower pressure, which means flash is slower and weaker than on an arm vein. Some providers compensate by advancing aggressively, which threads the catheter past the lumen or into the subclavian junction. Drop the angle, advance slowly, confirm with saline flush.
- Securement underestimated. The neck moves with breathing, swallowing, and head position changes. A standard arm-IV dressing is not enough. Use a strain-relief loop and reassess securement at every shift change.
This is exactly the kind of advanced technique covered in Level 2: The Craft, our advanced IV cannulation intensive. Level 2 builds on the foundational skills from Level 1: The Method and adds difficult-access techniques, including supervised practice on advanced peripheral sites under the observation of credentialed clinical instructors with active field experience.
Frequently asked questions
Is EJ IV access a central line?
No. EJ IV access uses a standard peripheral IV catheter inserted into the external jugular vein, which is a peripheral vein in the lateral neck. The catheter tip stays in the peripheral circulation, not in the superior vena cava or right atrium. That classification has implications for dwell time, infection control protocols, and scope of practice. EJ is a peripheral procedure performed within RN scope at most institutions; central lines are placed by physicians, advanced practice providers, or specially credentialed RNs.
Can RNs insert EJ IVs?
Yes, with the right credentials. The Infusion Nurses Society explicitly supports RN insertion of EJ peripheral IV catheters when the nurse has documented competency and institutional approval. Most state boards of nursing, including Arizona, defer to facility policy and demonstrated skill. You need three things in place: a state board position that allows it, an institutional protocol that authorizes your role to perform it, and individual competency documentation.
What is the success rate of external jugular cannulation?
Published data shows a 62% first-attempt success rate and 79% overall success across two attempts for junior clinicians, with a mean of 1.5 attempts per successful insertion and a mean cannulation time of 148 seconds. Experienced operators with structured training report higher rates, often above 80% on first attempt. Pediatric studies show success rates around 90%, suggesting the technique transfers across patient populations with appropriate training.
When should I choose EJ vs. ultrasound-guided peripheral IV?
Choose EJ when access is time-critical, the EJ is visible after positioning, and you have documented competency. Choose ultrasound-guided peripheral IV when you have time for the setup, the patient has accessible deeper veins, and you are credentialed for USGPIV. In a true emergency where peripheral access has failed and the patient is decompensating, EJ is often faster than setting up ultrasound. In a stable but difficult-access patient, USGPIV is usually the better first choice.
Is EJ IV access dangerous?
In trained hands, the complication rate is low. Published research reports a 4% overall complication rate, dominated by minor insertion-site swelling and catheter malposition. Serious complications such as arterial puncture, pneumothorax, and infection were not reported in the largest published case series. The risks that exist with internal jugular and subclavian access are functionally absent because the EJ sits well lateral to the carotid artery and the pleura.
How long can an EJ IV stay in?
EJ peripheral IV catheters are intended for limited dwell time. Most institutional protocols specify a maximum of 24 to 72 hours, with reassessment for an alternative access site at every shift change. The EJ is a bridge access, not a definitive solution. As soon as the patient is stable enough to allow placement of a more durable access (peripheral IV at a standard site, midline, or central line as clinically indicated), transition the patient and remove the EJ.
Ready to add EJ to your skill set?
If you are an experienced provider looking to add advanced peripheral access including EJ, ultrasound-guided IV, and difficult-access techniques to your skill set, Level 2: The Craft covers the methodology and provides supervised live-stick practice. Level 2 is built for providers who have foundational cannulation confidence and want to become the access provider their unit calls when nothing else is working. If you are still building that foundation, Level 1: The Method is where to start. Both courses are taught by credentialed clinicians with active field experience under a mastery-based curriculum where students advance when they demonstrate competence, not when the clock runs out. Enrollment is open, and pricing starts at $199 for Level 1.
VeinCraft Academy is a mastery-focused IV cannulation training program for healthcare professionals. All instruction is delivered by credentialed clinicians with active field experience. VeinCraft Academy is a RevivaGo Company.