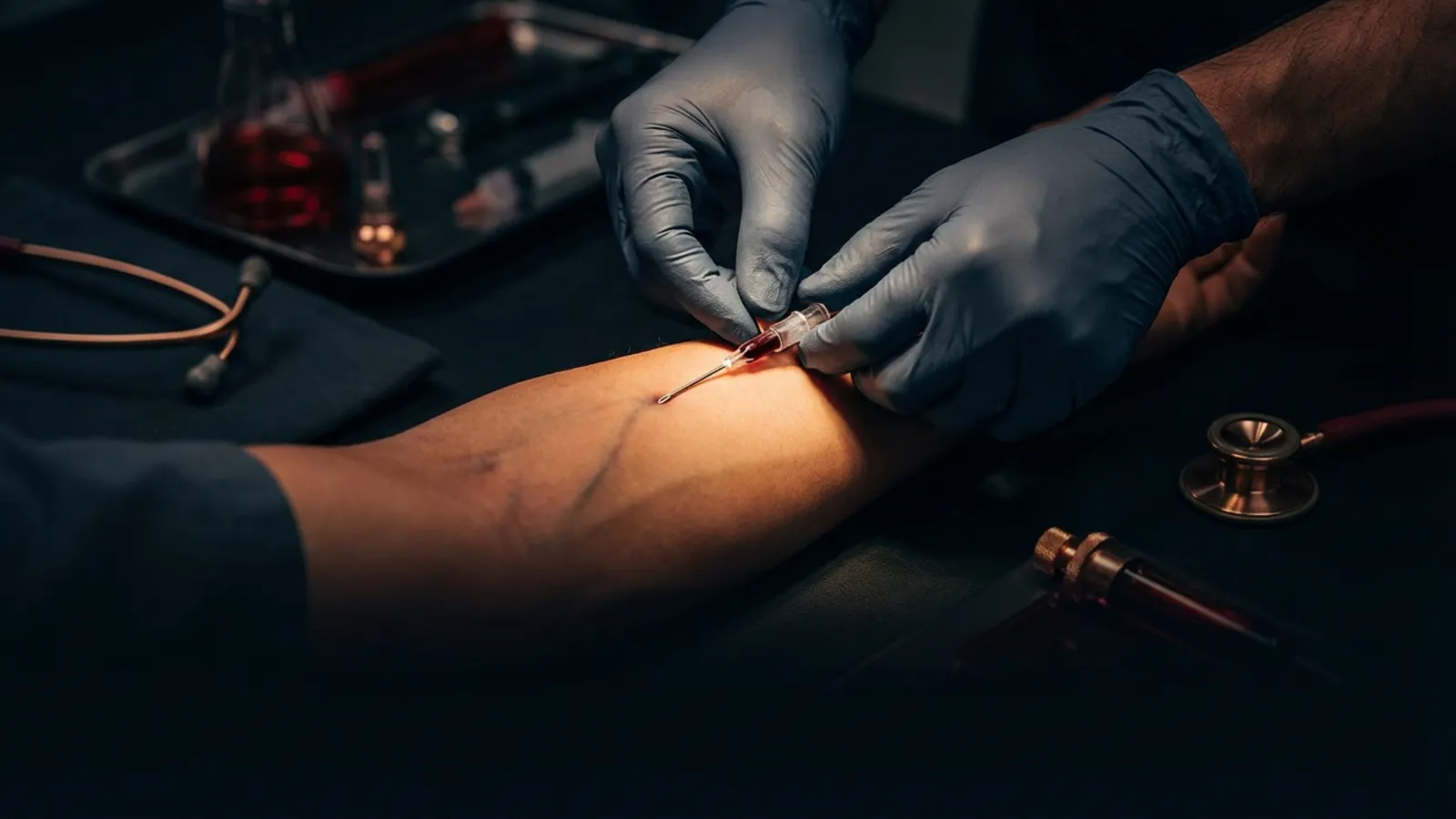
IV flash is the visible return of blood in the catheter's flashback chamber that confirms the needle tip has entered the vein lumen. Recognizing flash quickly and responding with the correct sequence of movements, lowering the angle, advancing slightly, and threading the catheter, is the difference between a successful IV start and a blown vein. According to the NCBI Bookshelf's Nursing Advanced Skills guide, flashback is the only reliable visual indicator that venous access has been achieved during peripheral IV cannulation.
Every provider who starts IVs knows the moment: you puncture the skin, you watch the chamber, and then either blood appears or it does not. What separates providers who consistently get clean starts from those who fumble through multiple attempts is not the puncture itself. It is what happens in the two to three seconds after flash appears. That window is where most IV failures actually occur.
What IV flash looks like
Flash is the appearance of blood in the flashback chamber (the small transparent reservoir at the base of the needle stylet) immediately after the needle tip enters the vein. Depending on the catheter type and gauge, you may see flash in two locations:
First flash (needle flash). Blood appears in the flashback chamber of the needle stylet. This confirms the needle bevel has entered the vein lumen. First flash happens fast, often within a fraction of a second of puncture.
Second flash (catheter flash). Blood appears between the catheter wall and the needle, visible as blood tracking up the catheter shaft. This confirms that the catheter tip, not just the needle tip, is inside the vein. Second flash is the more reliable confirmation that the catheter is positioned correctly for advancement.
Not every catheter design shows both types of flash clearly. Smaller-gauge catheters (22g, 24g) produce less visible flash because of lower blood flow volume. In dehydrated patients or those with low blood pressure, flash may appear slowly or as a small drop rather than a definitive rush of blood. Learning to recognize these subtle presentations is part of building reliable technique.
The correct response after flash
What you do in the two to three seconds after flash determines whether the IV succeeds or fails. This is where most providers, especially early in their careers, make the errors that lead to blown veins, through-and-through punctures, and failed threading.
See flash and pause. Do not keep advancing the needle at the same angle and speed. The moment you see blood return, your forward motion should stop briefly. This pause is measured in fractions of a second, not actual waiting. It is a deceleration, not a full stop.
Lower your angle. Drop the needle angle to nearly parallel with the skin surface, roughly 5 to 10 degrees. The vein runs horizontally beneath the skin. If you continue at your original insertion angle (typically 10 to 30 degrees), the needle will punch through the posterior wall of the vein. Lowering the angle aligns the needle path with the vein path.
Advance 2 to 4 millimeters. Push the entire unit (needle and catheter together) forward a small distance. This ensures that both the needle tip and the catheter tip are fully inside the vein lumen, not just the needle bevel. If you skip this step, the catheter tip may still be outside the vein when you try to thread it forward.
Stabilize and thread. Hold the needle stylet steady with your dominant hand. Use your thumb on the catheter hub to slide the catheter off the needle and into the vein. The catheter should advance smoothly with minimal resistance. If you feel resistance, do not force it. Resistance usually means the catheter tip is catching on a valve, the vein wall, or the catheter is not fully inside the lumen.
Remove the stylet and connect. Once the catheter is fully advanced to the hub, withdraw the needle stylet, apply pressure proximal to the catheter tip to prevent blood leakage, and connect your extension set or saline lock.
The float technique for difficult advancement
When standard catheter advancement meets resistance after flash, the float technique can save the stick. This is particularly useful for elderly patients with fragile veins and patients with small or tortuous vasculature.
After confirming flash, connect a prefilled saline flush syringe to the catheter hub (or to an already-connected extension set). Gently push saline while simultaneously advancing the catheter. The fluid opens the vein ahead of the catheter tip, reducing friction against the vessel wall and allowing the catheter to glide past minor obstructions like valves.
The float technique works because it creates a fluid column that distends the vein and essentially paves the path for the catheter. Providers who learn this technique report fewer post-flash threading failures, particularly in patients with small or fragile veins.
Common flash mistakes
Most IV failures do not happen at the puncture. They happen after flash, during the advancement phase. These are the errors that account for the majority of post-flash failures.
Advancing too far after flash. The most common mistake. You see flash, you are relieved, and you push forward with too much enthusiasm. The needle exits through the posterior vein wall, and now you have a through-and-through puncture. Blood appeared, then disappeared. The vein is blown.
Not lowering the angle. Continuing at the original insertion angle after flash sends the needle downward through the vein. The vein is a horizontal tube. Your approach must flatten to match it once you are inside.
Hesitating too long after flash. The opposite of advancing too fast. You see flash, freeze, and lose the moment. While you hesitate, the needle may shift slightly, the vein may spasm, or the patient may move. Flash is a signal to act, not to think. The correct response should be trained to the point of reflex.
Threading the catheter before the tip is inside the vein. If you advance the catheter before confirming that both the needle and catheter tips are inside the lumen (via that 2-4mm post-flash advance), the catheter folds against the outside of the vein wall. You feel resistance, push harder, and damage the vessel.
Ignoring partial flash. A small drop of blood rather than a definitive rush may indicate the needle bevel is partially inside the vein. The correct response is to lower the angle slightly and advance 1 to 2 millimeters until you see full flash. Withdrawing and restarting is premature at this point.
The psychology of flash recognition
Flash recognition is partly visual and partly reflexive. The visual component, seeing blood appear in the chamber, is straightforward. The reflexive component, responding with the correct motor sequence without conscious deliberation, is what separates confident providers from anxious ones.
When you are anxious, your central nervous system activation narrows your visual field, increases hand tremor, and slows your reaction time. Flash happens fast. If your stress response is running high, you may not register flash quickly enough, or you may overcorrect when you do see it.
This is why psychology-first IV training matters. Providers who have practiced the post-flash sequence enough times to make it automatic perform better under pressure than providers who are still thinking through each step consciously. The goal is not to eliminate the stress of the stick. It is to make the correct response so well-rehearsed that it executes even when your heart rate is elevated.
According to a 2023 study published in the Journal of PeriAnesthesia Nursing, 80.4% of nursing students report significant anxiety during IV interventions. That anxiety specifically degrades the fine motor control and rapid decision-making that the post-flash window demands. Building flash response into muscle memory through repeated practice is the most effective countermeasure.
How to practice flash recognition
You cannot develop reliable flash recognition by watching videos. You develop it by performing IV starts repeatedly in conditions that approximate real clinical practice.
Simulation models provide a controlled environment for initial practice. They let you see flash in a predictable context and rehearse the post-flash sequence without patient risk. But simulation flash feels different from real flash. The resistance, the speed of blood return, and the tactile feedback of the vein are all approximations.
Live-patient practice is where flash recognition becomes a real skill. On actual patients, flash varies. It can be fast or slow, obvious or subtle, abundant or barely visible. Each variation teaches your hands and eyes something simulation cannot.
Programs like VeinCraft Academy's Level 1: The Method build flash recognition through a structured progression: psychology-first instruction, simulation practice, and then supervised live-patient sticks where an instructor watches your post-flash response and corrects in real time. At $199, it compresses what might take months of on-the-job trial and error into a single focused day. Level 2: The Craft builds further with difficult access patients and ultrasound-guided technique at $299.
What does IV flash look like?
IV flash is the visible appearance of blood in the catheter's flashback chamber, confirming the needle tip has entered the vein. It typically appears as a sudden rush of dark red blood filling the small transparent reservoir at the base of the needle stylet. In smaller-gauge catheters or dehydrated patients, flash may appear as a slow trickle or a small drop rather than a definitive rush. Some catheter designs also show a second flash of blood tracking between the catheter wall and the needle, confirming the catheter tip itself is inside the vein.
What do you do after you see IV flash?
Immediately lower your insertion angle to nearly parallel with the skin (5 to 10 degrees), advance the entire needle-catheter unit 2 to 4 millimeters to ensure the catheter tip is inside the vein, then stabilize the needle and thread the catheter off the stylet into the vein. Do not continue advancing at your original angle after flash, as this causes through-and-through puncture of the posterior vein wall. The post-flash sequence should be practiced to the point of reflex.
Why do I get flash but the catheter won't thread?
The most common reason is that the catheter tip is not fully inside the vein lumen when you attempt to thread. This happens when you skip the 2-4mm post-flash advance or do not lower your angle sufficiently. Other causes include the catheter catching on a venous valve (try rotating the catheter slightly or using the float technique with a saline flush), a vein that has spasmed from tourniquet pressure or patient anxiety, or a vein that is too small for the selected catheter gauge. If threading fails after one gentle attempt, do not force it. Withdraw and restart at a new site.
Can you miss flash during IV insertion?
Yes. Flash can be missed if the flashback chamber is obscured by your grip, if the patient is severely hypotensive (reduced venous pressure produces minimal blood return), or if you are not watching the chamber at the moment of puncture. In very dehydrated patients, flash may be delayed or appear as a barely visible trickle. Providers who rely on tactile feedback (the subtle "pop" of venipuncture and the change in resistance as the needle enters the lumen) in addition to visual flash have higher success rates because they are not dependent on a single confirmation signal.
Flash recognition is a trainable reflex, not a talent. Every provider who starts IVs can develop the speed and accuracy to act on flash correctly, but it takes supervised repetition on real anatomy, not just video demonstrations. If you want to build flash technique into muscle memory through hands-on training with live patients, explore VeinCraft Academy's courses and see how mastery-based progression starting at $199 builds confidence that holds up under real clinical pressure.
VeinCraft Academy is a mastery-focused IV cannulation training program for healthcare professionals. All instruction is delivered by credentialed clinicians with active field experience. VeinCraft Academy is a RevivaGo Company.